What is Legionella pneumophila and how does it spread in water systems
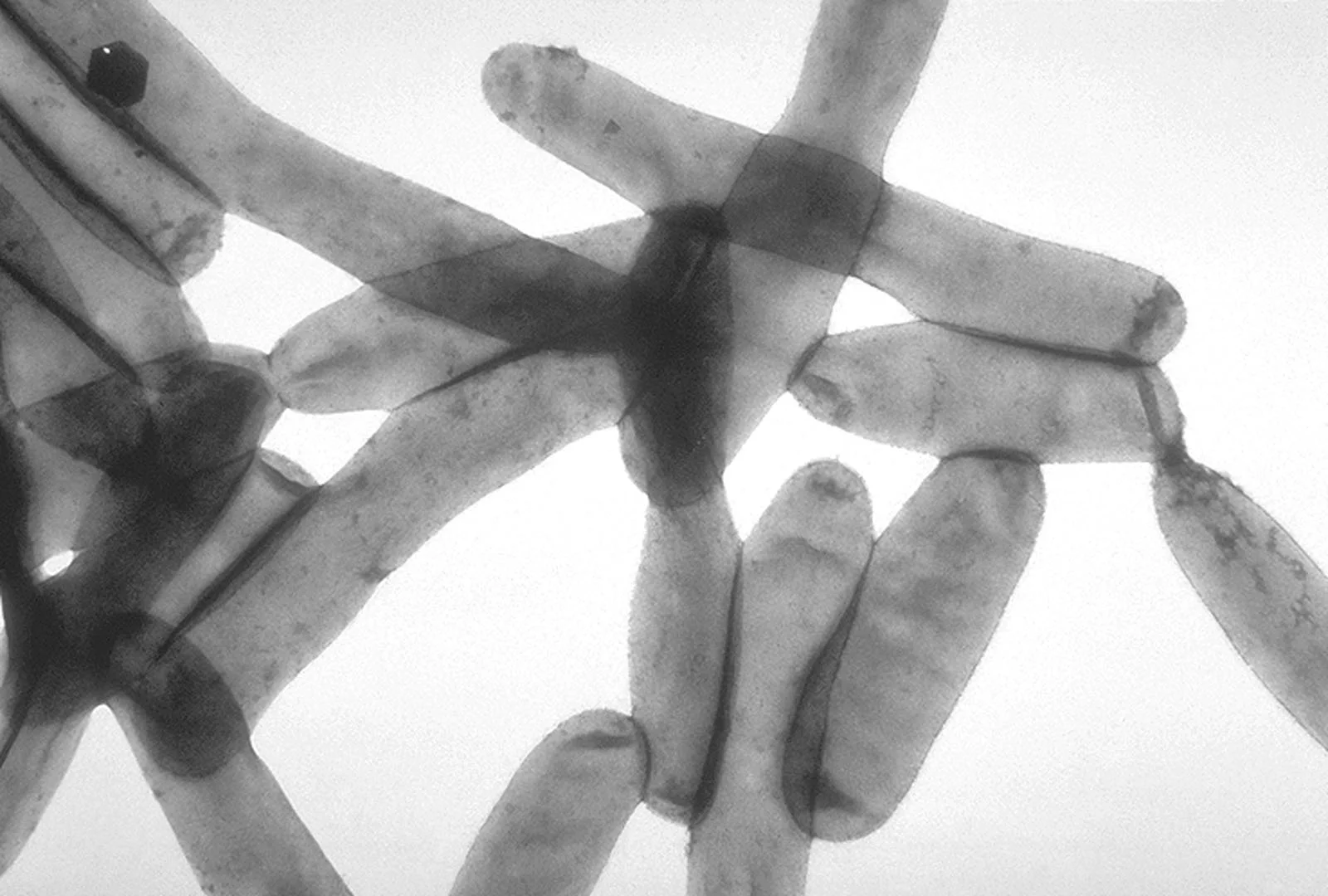
What is Legionella pneumophila
Legionella pneumophila is a bacterium that naturally occurs in water (e.g., lakes, rivers), mostly in low concentrations, but in man-made water systems, it can multiply significantly and subsequently cause illness – especially Legionnaires’ disease (a severe form of pneumonia) and sometimes the milder “Pontiac fever”.
Crucially, Legionella often “hides” and survives in systems:
- in biofilm (a slimy layer of microorganisms on the walls of pipes and equipment),
- in free-living protozoa, where it can multiply.
When it thrives in water systems
Legionella multiplies best at “lukewarm” temperatures:
- typically in the range of approximately 20–50 °C (optimum around 35 °C),
- practically, the most critical range is 25–45 °C – temperatures that are relatively common in buildings (mixed water, insufficiently heated hot water, overheating of cold water in distribution systems).
Growth and persistence are primarily supported by:
- water stagnation (dead legs, rarely used outlets),
- “water age” (water standing in the system for a long time),
- sediment and limescale,
- low disinfectant residual (where it should be present),
- biofilm and suitable conditions in pipes and equipment.
How it spreads: the transmission mechanism in brief
Legionella is typically not transmitted by drinking water, but by inhaling tiny droplets (aerosol) that contain the bacteria. It does not commonly spread from person to person. The most common “chain” of spread in water systems is as follows:
- System Colonization
– the bacteria enters the building (e.g., from the external water supply network or the environment) and attaches to areas where biofilm forms. - Amplification (Overgrowth)
– if conditions are met (temperature, stagnation, biofilm, sediment), the concentration in certain sections increases. - Aerosolization (Formation of tiny droplets)
– during the operation of certain equipment or systems, micro-droplets of water are formed and released into the air. - Human Exposure
– a person inhales the aerosol (or, exceptionally, water aspiration into the respiratory tract occurs – more commonly in healthcare facilities).

How to prevent Legionella in buildings (temperatures, flushing, maintenance, monitoring)
Legionella typically overgrows in buildings when there is lukewarm water, biofilm, and time (stagnation). Therefore, prevention rests on 4 pillars: correct temperature, minimal stagnation, regular maintenance, and parameter control.
Temperature regime: keep water out of the bacteria’s “comfort zone”
Most commonly recommended temperature control in domestic hot water (DHW)/cold water distribution systems:
- Hot Water (DHW): store at ≥ 60 °C, distribute so that it reaches the outlet at at least 50 °C (in some stricter operations, e.g., healthcare, 55 °C at the outlet within a specified time is also stated).
- Cold Water: maintain < 20 °C (practically, it’s a problem when cold water in the building “heats up” in shafts and long distribution lines).
- Legionella multiplies best at approximately 25–45 °C – precisely where water is found with poor circulation, long branches, or in rarely used sections.
Safety note: high temperatures increase the risk of scalding, which is why in practice, a hot distribution system is often combined with outlet safety measures (e.g., appropriate mixing/thermostatic elements depending on the type of operation). This is addressed by the designer and operator as part of the building’s operational regime.
Hygienic Flushing: stagnation is the most common trigger of the problem
Even with good heating temperatures, Legionella can persist in:
- “dead legs” (blind branches),
- rarely used outlets (guest restrooms, seasonal areas, warehouse facilities),
- long pipes with low flow.
Therefore, regular flushing and managing “water age” (the age of water) are important. For example, the CDC recommends for low-flow branches and dead legs at least weekly flushing as a practical measure (the specific frequency depends on the risk and the facility).
HSE also emphasizes that rarely used outlets should be flushed regularly.
Flushing is most effective where aerosol is actually generated (showers) and where there is long-term low usage (selected faucets, urinals, toilets in peripheral parts of the building).
Thermal Disinfection: when a system “reset” is needed
As an intervention (or periodic) measure, thermal disinfection is also used – flushing the system with high-temperature water under strict safety rules.
Example from guidance: flushing outlets with water ≥ 70 °C for at least 5 minutes, or ≥ 60 °C for at least 10 minutes, if 70 °C is not achievable, with emphasis on preventing scalding and controlling access to outlets during the intervention.
In practice, this always falls under the responsibility of a designated person/service, especially in public facilities.
Senzor company also has products in its portfolio that support hygienic flushing and disinfection functions.

Latest technologies and
optoelectronic precision

Long durability
of quality materials

Certified to
European standards

All our products are
manufactured in Slovakia


